Small practices struggle with rising costs and inconsistent reimbursements. Billing presents one of the biggest challenges, especially when limited staff and resources handle it in-house. Salaries, training, and software expenses quickly drain budgets, while errors and delays directly reduce revenue.
This is why many providers choose to outsource. Outsourcing promises greater efficiency, reduced errors, and improved collections. But one question always comes up first: How much do medical billing services actually cost?
In this guide, we break down pricing models, average costs, and actionable considerations to help small practices make informed decisions about investing in professional billing support.
What Are Medical Billing Services?
Medical billing services manage the financial operations of healthcare organizations. Their main function is to ensure providers receive prompt, accurate payments for the care they deliver.
These services typically involve claim submission, coding expertise, payment processing, and denial resolution. They oversee the entire billing cycle to minimize errors and maximize reimbursement rates.
Medical billing is also a key part of revenue cycle management. It connects front-end processes, such as patient registration, with back-end activities, such as collections and reporting. A well-managed billing system supports consistent cash flow and reduces administrative burden.
Curious about where billing fits in the larger healthcare picture? Let’s explore the full revenue cycle management process together.
Common Pricing Models for Medical Billing Services
Medical billing companies use different pricing structures based on the services offered and the practice’s needs. Understanding these models helps providers choose the best option for their situation.
Percentage-Based Pricing
Most billing companies use a common pricing model in which the provider pays a percentage of total collections.
Rates typically range from 4 percent to 10 percent. Most small practices fall between 5% and 8%.
The main advantage is that billing companies stay motivated to maximize collections. Their earnings depend on your revenue, so their goals align with yours.
Your costs may vary depending on how much you collect each month. If you bring in higher revenue, you pay higher billing fees.
Flat Fee Pricing
With flat-fee pricing, you pay a fixed monthly cost regardless of how much you collect. This model usually bases fees on claim volume or the scope of services you need.
You benefit from predictable costs, which helps with budgeting. You know exactly what you will pay each month.
However, this model may not always track performance. Whether your collections improve or decline, you pay the same fee.
Per Claim Pricing
This model charges providers a fixed fee per submitted claim. This approach suits practices with low claim volume or simple billing needs.
You gain transparency and control over costs, but you may not receive full revenue-cycle services, such as denial management or reporting.
Evaluate whether this model covers all the services you need before you choose it.
Average Cost of Medical Billing Services for Small Practices
Small practices seeking medical billing services often wonder what costs to expect. These costs can vary according to multiple factors, but there are general benchmarks that offer guidance.
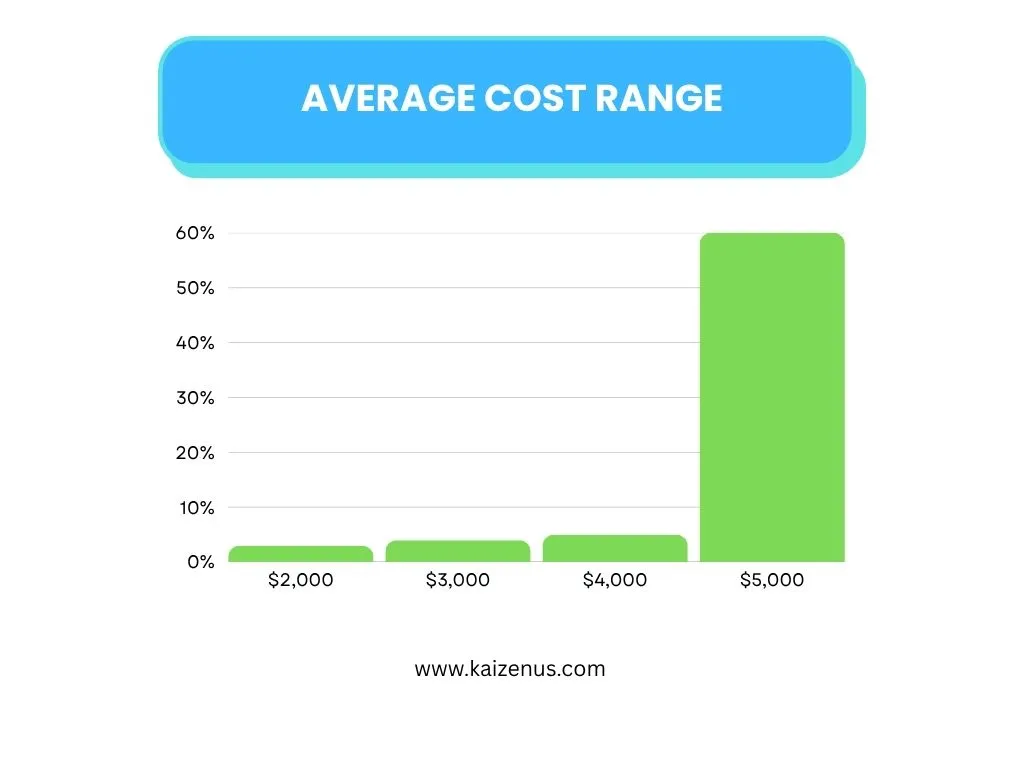
Most small practices spend between $1,000 and $5,000 per month on outsourced billing services. This range depends on claim volume, specialty, and complexity.
For percentage-based models, the typical range is 5% to 8% of collections. Practices with higher complexity or lower volume may see slightly higher rates.
Several factors influence pricing. Specialty plays a major role, as some fields require more complex coding and documentation. Claim volume also affects costs, with higher volume often resulting in better rates.
The level of service included is another key factor. Full-service billing, including coding, denial management, and reporting, will cost more than basic claim submission.
What Is Included in Medical Billing Service Fees
Medical billing service costs often span the entire billing cycle, so understanding what is included helps practices assess value, not just price.

Most billing services include insurance verification, which confirms patient coverage before providing services. This step minimizes claim denials and boosts accuracy.
Coding support remains vital. Precise coding ensures compliance and secures correct reimbursement.
Claim submission forms the heart of billing services. Accurate, prompt submissions maximize approval rates.
Denial management appears in most service packages. This includes flagging denied claims, correcting issues, and resubmitting them for payment.
Reporting and analytics reveal performance insights. Practices track metrics such as collections, denial rates, and accounts receivable days.
Some providers may charge extra for certain services, so it is crucial to carefully review the scope and clarify costs in advance to avoid unexpected expenses.
Hidden Costs to Watch Out For
Not all billing costs are immediately visible. For example, some providers include additional charges that can increase overall expenses.
One such example is setup fees, which are common when starting with a new billing company. These typically range from $200 to $1,000 and cover onboarding and system integration.
In addition, credentialing charges may apply if the billing company assists with provider enrollment, such as a $100 per-provider application fee or a flat fee per project.
Software costs can also be a factor. For instance, some companies require practices to use specific systems, pay licensing fees, or purchase additional user seats to access them.
Furthermore, clearinghouse fees, such as $0.25 per claim, may be billed separately for claim processing.
Another area to consider is reporting add-ons. For example, advanced analytics and custom reports may not be included in the base price, so if you require detailed performance metrics or specialized financial summaries, these could represent extra costs.
By remaining aware of these hidden costs, practices can avoid surprises and make informed decisions.
In-House Billing vs Outsourced Medical Billing Cost Comparison
Understanding the difference between in-house and outsourced billing costs is essential for small practices.
| Salaries for staff | Percentage of collections |
| Training costs | Included |
| Software expenses | Included |
| Higher overhead | Lower overhead |
In-house billing requires hiring and training staff, investing in software, and managing ongoing expenses. It also increases administrative burden.
When considering outsourced billing, compare service providers and negotiate performance-based agreements. Clarify which expenses are included and set clear communication protocols with your provider.
For most small practices, outsourcing is more cost-efficient and easier to manage.
Is Outsourcing Medical Billing Worth the Cost?
Outsourcing medical billing can be a strategic decision that drives substantial financial improvement, not just direct cost savings.
Professional billing teams reduce errors, resulting in fewer claim denials. This increases the likelihood of receiving full reimbursement.
When claims are processed faster, payments arrive sooner, and cash flow improves.
Outsourcing also reduces the workload on in-house staff. This allows providers to focus more on patient care rather than on administrative tasks.
While many practices find that outsourcing’s return on investment outweighs its costs, it is helpful to examine the detailed benefits of medical billing outsourcing to better understand this.
How to Choose the Right Medical Billing Company Based on Cost
Selecting the right medical billing company requires careful consideration, especially when evaluating costs alongside quality.
Firstly, avoid choosing the cheapest option. Inferior billing performance will cause higher denial rates and lost revenue.
Secondly, prioritize value. Demand companies with robust reporting, high clean claim rates, and proven experience.
Thirdly, insist on transparency. A dependable billing company must clearly explain its pricing and services.
Finally, rely on performance metrics and client feedback to make your decision.
Why Small Practices Choose Kaizen Systems?
Kaizen Systems attracts small practices by delivering tangible benefits such as performance enhancement and transparency, along with comprehensive billing and revenue cycle support tailored to smaller providers.
Kaizen’s certified billing and coding professionals ensure process accuracy. This reduces errors and improves claim approval rates.
The team lowers denials with proactive strategies and detailed analysis. This improves collections and speeds payments.
Transparent reports help practices track performance and identify opportunities for improvement.
By combining expertise, technology, and a results-driven approach, Kaizen helps small practices achieve stronger financial outcomes.
FAQs
Most small practices pay between $1,000 and $5,000 per month, depending on claim volume and services.
When it comes to rate structures, you’ll typically see rates ranging from 5 percent to 8 percent of collections.
In most cases, outsourcing is more cost-efficient due to lower overhead and better performance.
However, did you know some providers charge extra for setup, software, or reporting? Take a close look at the pricing structure to avoid surprises.
When choosing a billing service, look beyond cost and seek value, transparency, proven experience, and reliable performance metrics for lasting success.
Final Words
Medical billing services cost depend on practice size, claim volume, and service level. Most small practices save more by outsourcing billing than by handling it themselves.
Outsourcing reduces costs, improves accuracy, lowers denials, and speeds up reimbursement. These effects improve cash flow and financial results.
Therefore, choose a billing partner with transparent pricing, strong reporting, and proven results.
Take the next step to optimize your billing: connect with a partner who specializes in supporting small practices and delivers proven financial results.



