Unpaid claims don’t just sort themselves out. In many cases, practices send out claims and then move on, but without proper follow-up after submission, they end up leaving money on the table. As a result, that is exactly where revenue starts slipping through the cracks.
When you let follow-up slide, your AR starts piling up. Unworked claims, ignored denials, and payment delays all add up fast. This hits your cash flow hard and can make it tough to cover day-to-day expenses or invest back into your practice.
If you don’t stay on top of AR follow-up, you’ll end up writing off more claims and losing revenue you’ve already earned. AR follow-up isn’t just busywork. It’s a core part of your revenue cycle management that directly affects how much you actually collect and how stable your finances are.
Let’s break down what AR follow-up really means and how you can use it to boost your revenue.
What Is AR Follow-Up in Medical Billing?
Accounts receivable in medical billing means the money a healthcare practice is owed for services already provided. These are claims sent but not yet paid by insurance companies or patients.
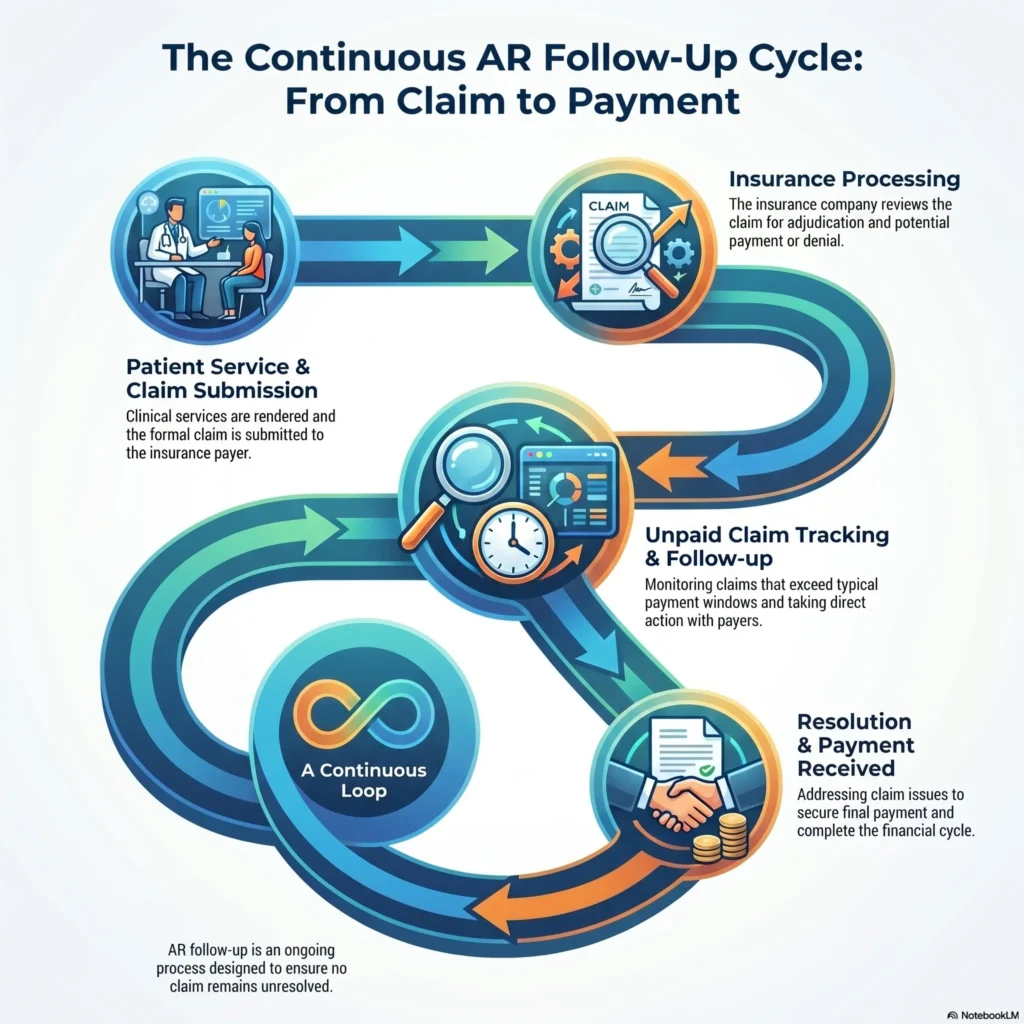
AR follow-up means keeping track of unpaid claims and working to get them paid. This involves checking claim status, spotting problems, and fixing them quickly. Without good follow-up, claims can stay unpaid for a long time. This causes more denials, delays, and lost money. In short, A clear AR process makes sure claims are reviewed and handled until payment comes in.
Why AR Follow-Up Is Important?
AR follow-up is what keeps your revenue steady. In fact, it helps you catch simple mistakes before they turn into unpaid claims.
When you follow up consistently, you get paid faster. As a result, you can spot delays early and stop claims from aging out before you can collect. This way, revenue does not slip through your fingers. On the other hand, if you let claims sit, they get forgotten or written off, and that’s money lost.
Staying on top of follow-up boosts your cash flow and keeps your AR under control, which is key for financial stability.
Understanding AR Aging in Medical Billing
AR aging shows you how long claims have been unpaid. By sorting claims by how old they are, you can decide which ones to focus on first.
Aging Buckets
0 to 30 days
31 to 60 days
61 to 90 days
90 plus days
Each group shows how long a claim has been waiting for payment. As a general rule, the older the claim, the harder it is to collect. At first, claims in the 0–30 day group are usually still being processed. However, once they move into the older groups, the chances of denial or being written off increase significantly. Therefore, by tracking AR aging, your billing team can zero in on high risk claims and take action before it is too late.
The AR Follow-Up Process
A good follow-up process makes sure no claim gets missed. Every step focuses on spotting problems quickly and fixing them.
Step 1: Identify Unpaid Claims
Start by pulling your AR reports and flagging any claims that haven’t been paid when they should have been.
Step 2: Verify Claim Status
Check each claim’s status using insurance websites or your billing service. You want to know if it’s still waiting, denied, or paid.
Step 3: Analyze Denial or Delay Reasons
If a claim is delayed or denied, find out why. Usually, it’s because of a coding mistake, missing information, or a problem with eligibility.
Step 4: Take Corrective Action
Once you know the problem, fix it by correcting errors, resubmitting the claim, or sending an appeal.
Step 5 Document Follow-Up Activity
Make sure you record every step you take. This helps you keep track of what’s done and hold everyone responsible.
Common Issues Found During AR Follow-Up
AR follow-up helps you spot patterns that drain your revenue. Catching these issues early is the first step to tightening up your billing process.
Claim denials are one of the most common problems. For example, a claim may be denied due to missing prior authorization in medical billing, which could have been avoided with careful verification before submission. Many of these denials can be prevented by identifying and addressing underlying causes early. You can explore this further in our guide on how to reduce claim denials in medical billing.
Underpayments are another problem. Sometimes, payers pay less than expected because of coding errors or contract problems. Missing paperwork can delay payments or cause claims to be denied. If your records aren’t complete, it’s hard to support your claims.
Coding mistakes happen often during follow-up. They can affect your payments and cause compliance problems. Regular reviews through a medical billing audit process help you find and fix these issues. Insurance delays can slow down the whole process. If you don’t follow up regularly, you might not notice these delays until it’s too late.
How AR Follow-Up Impacts Revenue
AR follow-up helps you resolve unpaid claims quickly by spotting and fixing problems right away. This means you get paid faster, and your finances improve.

Good follow-up leads to faster payments. Claims get settled quickly, cutting down the time between service and payment. It also helps reduce AR days in medical billing. When you manage unpaid claims well, you keep your receivables under control. Better follow-up means you collect more payments and improve your clean claim rate in medical billing. That puts more money in your pocket.
When your income is steady, your financial stability improves a lot. Practices that focus on AR follow-up are better able to pay bills and plan ahead. Good follow-up takes steady effort and a clear process.
Here are some best practices I’ve seen work to boost efficiency and results.
Prioritize Older Claims
Focus on the oldest claims first. The longer they wait, the harder they are to collect. Keep a regular follow-up schedule.
Stick to a regular schedule for reviewing and working on your AR. That way, claims don’t fall through the cracks.
Use Accurate Documentation
Keep your paperwork clear and complete, supported by insurance eligibility verification in medical billing. It speeds up claim processing and stops you from chasing the same claim repeatedly.
Track Key Metrics
Watch your key numbers so you can see where to improve and track your progress.
Train Billing Staff
Make sure your billing team is well-trained. They will handle difficult issues and work with insurance companies better to track in AR Follow-Up. Tracking the right numbers gives you real insight into how your AR is doing and helps you make better decisions.
Days in AR tells you how long it’s taking to get paid. The lower, the better. Collection rate shows what percentage of your expected payments you’re actually bringing in. The denial rate tells you how many claims are getting kicked back. If it’s high, you’ve got some billing issues to sort out.
First-pass resolution rate shows how many claims get paid the first time around, without extra work. The higher this number, the smoother your process will be.
How Outsourced Medical Billing Improves AR Follow-Up?
Outsourcing your AR follow-up can really ramp up your efficiency and results. You get a team that’s focused just on managing your receivables and clearing up issues. Experienced billers know what payers want and can handle the tough cases, which means your claims get resolved faster. Outsourced medical billing services also give you better tracking and reporting, so you can see exactly how you’re doing and spot trends right away.
A recent industry report supports the effectiveness of specialized AR management, indicating that practices utilizing outsourced billing services have reduced their average days in accounts receivable by 23% compared to those managing billing in-house (Medical Group Management Association, 2022).
At Kaizen Systems, our medical billing services and revenue cycle management solutions are designed to support small healthcare practices by providing consistent, reliable AR follow-up as part of a broader billing approach.
Frequently Asked Questions
AR follow-up is the process of tracking unpaid claims and taking action to secure payment from insurance companies or patients.
It ensures timely payments, reduces revenue loss, and improves overall cash flow.
They are time-based categories that show how long claims have been unpaid, such as 0-30 days and 90+ days.
By following up regularly, correcting errors quickly, and improving billing accuracy.
Yes, outsourcing provides dedicated teams, faster resolution, and better tracking of unpaid claims.
Final Thoughts
Bottom line is that AR follow-up is a must if you want to recover unpaid revenue and keep your finances steady. If you skip it, claims go unresolved, and you lose money you’ve already earned.
Consistent follow-up is what really moves the needle on AR days, collection rates, and cash flow. Track every claim, fix errors fast, and don’t let anything slip by. That’s how you win at AR follow-up.
If your receivables are piling up or payments keep getting delayed, now’s the time to tighten up your follow-up process. Team up with medical billing experts for small practices to take control of your AR.



