Healthcare providers face constant pressure to maintain steady cash flow while delivering quality patient care. Yet many medical practices struggle with claim denials, delayed reimbursements, and administrative inefficiencies that slow down the billing process.
One of the most important metrics for evaluating billing performance is the clean claim rate in medical billing. A strong, clean claim rate means that claims are submitted the first time correctly and move through the payer system without delays or corrections. When practices improve this metric, they reduce claim denials, accelerate reimbursements, and strengthen overall revenue cycle performance.
Understanding how clean claims work and how to improve them is essential for any practice that wants to optimize financial operations and maintain stable revenue.
What Is a Clean Claim in Medical Billing
A clean claim in medical billing is one submitted to an insurance payer with complete and accurate information. It contains all the required patient details, correct medical codes, and supporting documentation needed for processing. Because the claim is accurate and complete, the payer can review and process it without requesting additional information or corrections.
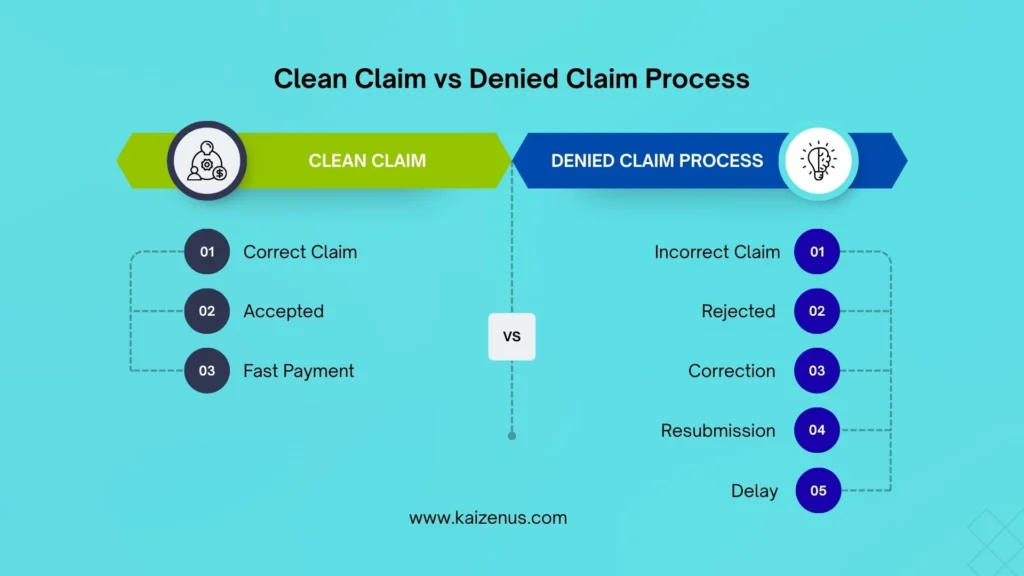
A clean claim typically includes accurate patient demographics, correct insurance details, proper diagnosis and procedure codes, and complete provider documentation. When these elements are submitted correctly, the claim moves smoothly through the payer’s system and reaches reimbursement faster.
Clean claims are critical to maintaining an efficient billing workflow. When claims contain errors or missing information, they are often rejected or denied by the payer. This forces billing teams to spend additional time correcting the claim and resubmitting it, which delays payment and increases administrative workload.
By focusing on clean claims from the beginning, medical practices can reduce unnecessary delays and maintain a more efficient billing process.
What Is Clean Claim Rate
The clean claim rate measures the percentage of claims that are accepted by payers without requiring corrections or additional information. It is one of the most widely used medical billing KPIs because it directly reflects the efficiency and accuracy of the billing process.

The formula for calculating the clean claim rate is simple.
Clean Claim Rate =
Clean Claims Submitted ÷ Total Claims Submitted × 100
For example, if a medical practice submits 1,000 claims in a month and 950 are accepted without issue, the clean claim rate would be 95%.
This metric provides valuable insight into the effectiveness of a practice’s billing operations. A higher clean claim rate means fewer errors during claim submission, fewer denials, and faster reimbursement cycles. A lower rate indicates that the practice may be experiencing problems with coding accuracy, patient information, eligibility verification, or documentation quality.
Regularly monitoring the clean claim rate helps healthcare administrators identify billing issues early and take corrective action before they significantly impact revenue.
Clean Claim Rate Benchmark in Industry
Healthcare organizations often rely on industry benchmarks to measure billing performance. These benchmarks provide a reference point that allows practices to evaluate whether their billing processes are performing efficiently.
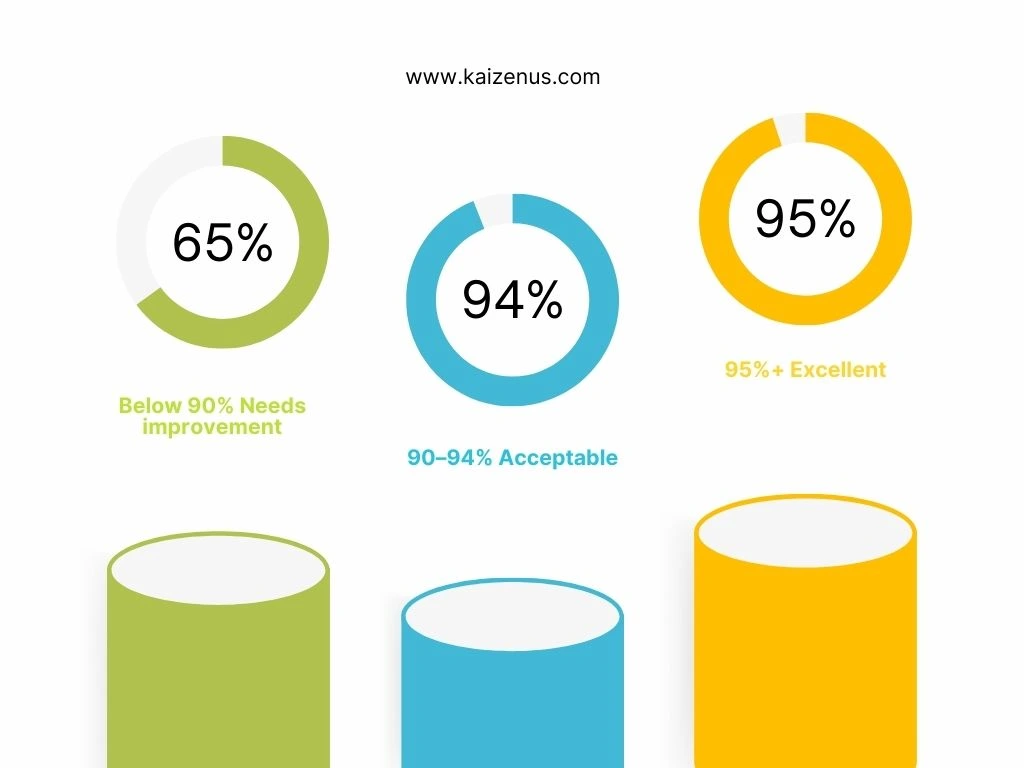
In most healthcare organizations, a clean claim rate of 95% or higher is considered excellent. Practices operating within this range typically have strong billing workflows, accurate coding practices, and reliable front-end data collection processes.
A clean claim rate of 90-94 percent is generally considered acceptable. While this range indicates reasonable performance, there may still be opportunities to improve processes and reduce minor errors that cause claim rejections.
When the clean claim rate falls below ninety percent, it usually signals deeper operational issues within the billing workflow. Common causes include inaccurate patient information, coding errors, missing documentation, or poor eligibility verification processes.
High-performing billing teams consistently maintain strong clean claim rates by implementing structured workflows, using modern billing technology, and closely monitoring payer requirements. By doing so, they ensure that most claims are processed successfully on the first submission.
Common Reasons Claims Are Rejected or Denied
Even experienced medical practices encounter claim rejections and denials. These issues often arise from preventable errors within the billing workflow. Understanding the most common causes helps practices take steps to reduce denials and improve clean claim performance.
Incorrect Patient Information
Patient demographic errors are one of the leading causes of claim rejections. Mistakes such as incorrect date of birth, inaccurate insurance identification numbers, or incomplete patient details can prevent claims from being processed correctly.
These errors often occur during patient registration or data entry. When patient information is not carefully verified at the front desk, the mistake travels through the entire billing process and ultimately results in a claim rejection.
Coding Errors
Medical coding plays a major role in claim accuracy. Incorrect diagnosis codes, mismatched procedure codes, or missing modifiers can trigger payer rejections. Coding errors may occur when documentation is unclear or when staff are unfamiliar with updated coding guidelines.
Ensuring accurate coding requires strong collaboration between providers, coders, and billing teams. Proper documentation and regular coding audits can significantly reduce these types of errors.
Missing Documentation
Insurance payers often require detailed documentation to support the services billed in a claim. When clinical notes are incomplete or supporting documents are missing, the payer may reject the claim or request additional information.
Incomplete documentation delays the reimbursement process and adds administrative work for billing staff, who must gather the required information and resubmit the claim.
Eligibility Verification Issues
Insurance eligibility verification is another critical step in the revenue cycle. When staff fail to confirm patient coverage before the appointment, claims may be submitted for services that are not covered by the patient’s insurance plan.
This often leads to claim denials that could have been avoided through proper verification during the scheduling or registration process.
Authorization Problems
Many insurance plans require prior authorization for certain procedures or treatments. If authorization is not obtained before the service is performed, the payer may deny the claim even if the service was medically necessary.
Ensuring that authorization requirements are reviewed and completed before treatment can prevent these avoidable denials.
How Clean Claim Rate Impacts Practice Revenue
A strong, clean claim rate directly improves the financial stability of a medical practice. When claims are submitted accurately and processed quickly, the entire revenue cycle becomes more efficient.
First, clean claims lead to faster reimbursements. Because the payer does not need to request corrections or additional information, the claim moves through the payment process without delays.
Second, clean claims reduce administrative workload. When billing teams spend less time correcting errors and resubmitting claims, they can focus on more valuable activities such as denial management and revenue analysis.
Third, a higher clean claim rate reduces the number of claim resubmissions. Each denied claim requires additional staff time to investigate the issue, correct the error, and resubmit the claim. By preventing these errors from occurring in the first place, practices save both time and operational costs.
Most importantly, improving the clean claim rate strengthens overall revenue cycle management performance. It allows practices to maintain consistent cash flow, reduce financial uncertainty, and operate more efficiently.
Strategies to Improve Clean Claim Rate
Improving the clean claim rate requires attention to several areas of the billing process. Healthcare organizations that focus on accurate data collection, proper coding practices, and effective billing workflows can significantly reduce claim errors.
Improve Front End Patient Data Collection
Accurate patient information is the foundation of clean claims. Front desk staff should verify patient demographics, insurance details, and contact information during every visit.
Using digital registration tools and verification systems can help ensure that patient data is collected accurately and consistently.
Ensure Accurate Medical Coding
Medical coding accuracy plays a critical role in claim acceptance. Practices should employ certified coders or provide ongoing coding training to staff members who handle coding responsibilities.
Regular coding audits can help identify coding error patterns and ensure that claims comply with current payer guidelines.
Verify Insurance Eligibility Before Visits
Eligibility verification should be performed before every patient appointment. Confirming coverage details helps prevent claims from being submitted to inactive insurance plans or plans that do not cover the requested services.
This simple step significantly reduces claim rejections related to insurance coverage issues.
Use Claim Scrubbing Technology
Modern billing software often includes claim scrubbing tools that automatically review claims for potential errors before submission. These systems check for missing information, incorrect codes, and formatting issues.
By identifying problems early, claim scrubbing technology allows billing teams to correct errors before the claim reaches the payer.
Train Billing Staff Regularly
Billing regulations and payer requirements change frequently. Regular training ensures that billing staff remains up to date with new coding rules, documentation requirements, and claim submission guidelines.
Well-trained staff are more likely to identify errors before claims are submitted, which helps maintain a higher clean claim rate.
How Professional Medical Billing Services Improve Clean Claim Rates
Many healthcare practices choose to work with professional billing companies to improve claim accuracy and strengthen their revenue cycle operations. Specialized billing teams bring experience, technology, and structured workflows that help reduce billing errors.
Professional billing teams review claims carefully before submission to ensure accuracy. They use advanced billing software and automated verification tools to detect errors that might otherwise lead to claim rejection.
Experienced billing professionals also monitor payer policies and coding updates to ensure compliance with current regulations. This helps prevent avoidable denials caused by outdated billing practices.
Another advantage of working with a dedicated billing partner is improved denial management. When claims are denied, experienced billing teams analyze denial patterns and implement solutions that prevent the same errors from recurring.
At Kaizen Systems, our medical billing specialists focus on improving claim accuracy, strengthening documentation processes, and optimizing revenue cycle performance for healthcare providers.
By applying proven billing strategies and modern technology, we help practices maintain strong clean claim rates and achieve faster reimbursements.
FAQs
A clean claim is a medical claim submitted to an insurance payer with accurate patient information, correct CPT and ICD codes, and complete documentation. Because the claim has no errors or missing details, it can be processed without corrections or resubmission.
A good clean claim rate benchmark is 95 percent or higher. Rates between 90 and 94 percent are acceptable, while anything below 90 percent usually indicates billing errors or workflow issues.
Clean claim rate measures billing efficiency. A higher rate means fewer claim denials, faster reimbursements, and improved cash flow for medical practices.
Practices can improve clean claim rate by verifying patient information, checking insurance eligibility, using accurate medical coding, and reviewing claims before submission.
Low clean claim rates are usually caused by patient data errors, coding mistakes, missing documentation, eligibility issues, or missing prior authorizations.
Final Thoughts
Improving the clean claim rate in medical billing is one of the most effective ways to reduce claim denials, accelerate reimbursements, and strengthen a medical practice’s financial health. When claims are accurate and complete the first time they are submitted, providers spend less time fixing billing errors and more time focusing on patient care.
Practices that prioritize accurate patient data, proper coding, eligibility verification, and strong billing workflows often achieve significantly higher clean claim rates. These improvements not only reduce administrative workload but also create a more stable and predictable revenue cycle.
If your practice is experiencing frequent claim denials or delayed payments, it may be time to evaluate your billing processes. Partnering with experienced billing professionals can help streamline operations, improve claim accuracy, and support long-term financial success.



