Many healthcare providers assume that medical billing and revenue cycle management mean the same thing. In reality, they represent different parts of the financial process that keep a medical practice running smoothly.
Medical billing focuses on submitting insurance claims and ensuring providers receive payment for services. Revenue cycle management, often called RCM, covers the entire financial journey of a patient encounter.
Understanding the difference between medical billing and revenue cycle management helps healthcare organizations identify gaps in their financial workflow.
When practices rely only on billing without managing the full revenue cycle, they often face claim denials, delayed reimbursements, and hidden revenue loss.
In this Blog, we will explore the difference between the RCM and medical billing.
What Is Medical Billing
Medical billing refers to the process of translating healthcare services into insurance claims and ensuring providers receive reimbursement for the care they deliver. It is one of the most visible administrative functions within healthcare revenue operations.
Billing teams work closely with coders and clinical staff to submit accurate claims to insurance companies and government payers.
Claim Submission and Processing
One of the primary responsibilities of medical billing is preparing and submitting claims to insurance companies. After a patient receives medical care, the services must be coded properly and entered into the billing system. The claim is then transmitted to the payer for review and payment determination.
Experienced billers know that claim accuracy at this stage directly affects the speed of reimbursement. Even a small mistake in patient demographics, insurance information, or procedure coding can trigger claim rejections or delays.
Payment Posting and Reconciliation
Once the insurance company processes the claim, payments are issued and must be posted into the practice management system. Payment posting helps the practice understand which portion of the claim has been paid by insurance and which amount remains the patient’s responsibility.
This step also allows billing teams to identify underpayments or discrepancies. When payments do not match the contracted reimbursement rates, the billing team investigates the issue and takes corrective action.
Denial Management
Claim denials are a common challenge in medical billing. When a claim is rejected or denied by an insurance payer, the billing team reviews the denial reason and determines the appropriate next step.
A skilled billing professional analyzes denial codes, corrects errors, and resubmits claims when possible. Effective denial management prevents revenue loss and improves the practice’s overall claim acceptance rate.
What Is Revenue Cycle Management
Revenue Cycle Management is a comprehensive financial process that begins before a patient even receives medical care and continues until the final payment is collected. While medical billing focuses mainly on claim processing, revenue cycle management oversees the entire financial workflow of a healthcare organization.
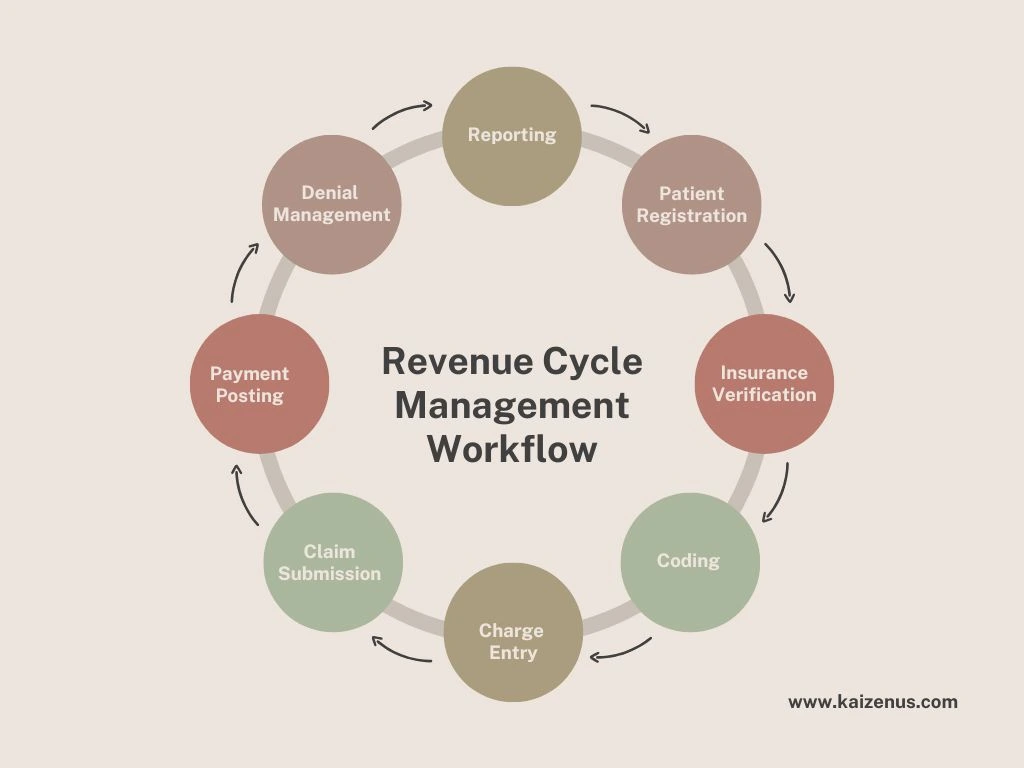
Patient Registration and Insurance Verification
The revenue cycle starts with patient registration. Accurate patient information is essential because errors at this stage can create billing complications later in the process. Staff members collect demographic data, verify insurance eligibility, and confirm coverage details before the appointment.
Insurance verification helps prevent claim denials related to coverage issues, inactive policies, or incorrect payer information. When verification is handled properly, practices reduce administrative rework and improve claim success rates.
Medical Coding and Charge Capture
Medical coding is another critical component of revenue cycle management. Certified coders translate clinical documentation into standardized diagnosis and procedure codes. These codes communicate the services performed during a patient visit.
Charge capture ensures that every billable service is recorded and submitted for reimbursement. Missing charges or incomplete documentation can lead to significant revenue leakage for healthcare providers.
Claim Submission, Payment Posting, and Denial Management
These steps overlap with traditional medical billing but are managed within the broader RCM framework. Claims are submitted to payers, payments are posted, and denials are analyzed to recover lost revenue.
In a well structured revenue cycle system, these processes are continuously monitored. Analytics and reporting tools help identify recurring billing errors and operational inefficiencies.
Reporting and Financial Analytics
Revenue cycle management also includes financial reporting and performance analysis. Healthcare administrators rely on revenue cycle data to evaluate metrics such as clean claim rate, denial rate, and average days in accounts receivable.
These insights allow practices to improve operational efficiency, strengthen compliance, and maintain a predictable revenue stream.
Key Differences Between Medical Billing and RCM
Although medical billing and revenue cycle management are closely connected, their scope and responsibilities differ significantly. Billing is one part of the larger revenue cycle.
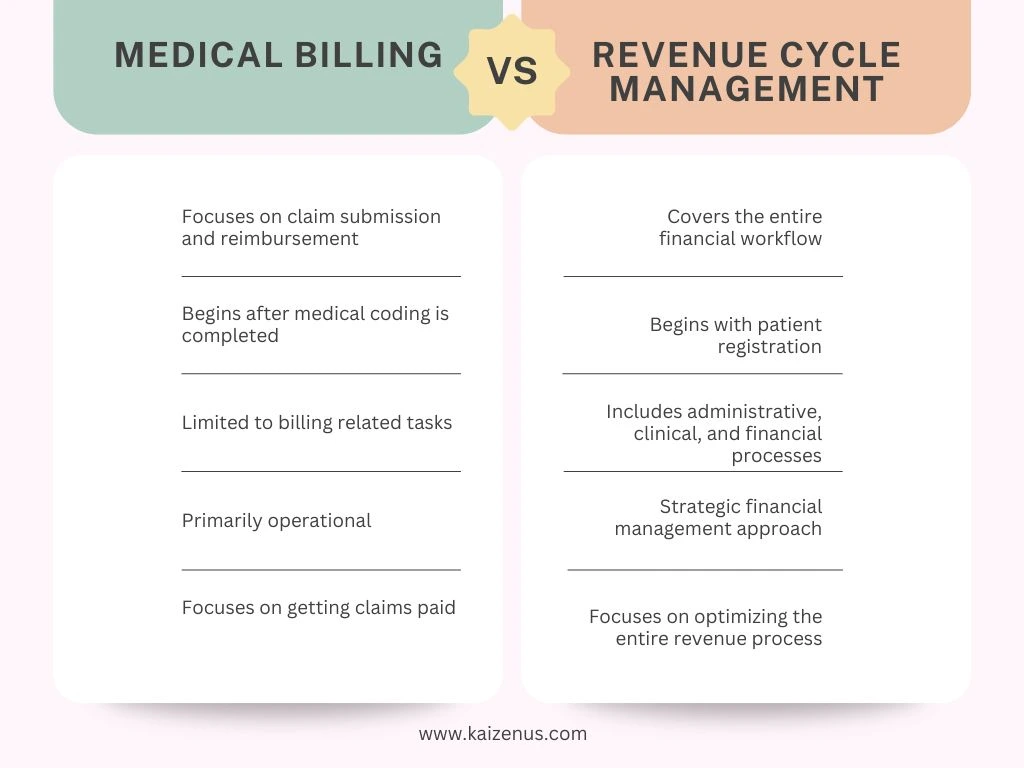
Scope of Responsibilities
Medical billing primarily focuses on administrative tasks related to claims. Billers prepare claims, communicate with insurance companies, and follow up on unpaid accounts. Their work is essential but limited to the claim reimbursement stage.
Revenue cycle management extends far beyond billing. It includes patient intake, insurance verification, coding accuracy, compliance monitoring, and financial reporting. Because it covers the entire patient financial journey, RCM provides deeper control over practice revenue.
Strategic Impact on Practice Revenue
Another key difference lies in the strategic role of RCM. Medical billing addresses individual claims, while revenue cycle management focuses on improving overall financial performance.
Through analytics and workflow optimization, RCM helps healthcare organizations reduce denial rates, increase clean claim submissions, and maintain steady cash flow.
Why Small Practices Need Full RCM?
Many small and mid-sized healthcare practices rely solely on basic billing services. While billing ensures claims are submitted and payments are collected, it does not address deeper operational problems that affect revenue stability.
Revenue Leakage and Missed Charges
Without a full revenue cycle strategy, practices often experience revenue leakage. Missing documentation, incomplete charge capture, or coding inaccuracies can result in services that never get billed.

Over time, these small gaps accumulate, resulting in significant financial losses for healthcare providers.
Delayed Reimbursements
Another challenge occurs when claims are repeatedly rejected or delayed. When billing teams focus solely on claim submission without analyzing the root causes of denials, the same errors continue to occur.
Revenue cycle management introduces proactive monitoring systems that identify patterns in claim rejections and correct them before they impact cash flow.
Improved Financial Visibility
RCM provides healthcare administrators with greater visibility into financial performance. Through detailed reporting and revenue analytics, practices can monitor their collection rates, denial trends, and reimbursement timelines.
This level of insight helps leadership make informed decisions about staffing, compliance, and operational improvements.
When Should a Practice Upgrade to RCM Services
Healthcare practices often realize the need for full revenue cycle management after experiencing persistent billing challenges. Recognizing these warning signs early can prevent financial instability.
Frequent Claim Denials
A high denial rate is one of the clearest indicators that the revenue cycle process needs improvement. When claims are repeatedly rejected due to coding errors, eligibility issues, or missing documentation, the practice spends excessive time correcting and resubmitting claims.
Delayed Payments
Slow reimbursements can strain a practice’s financial stability. If payments consistently take longer than expected, the issue may stem from inefficient billing workflows or incomplete insurance verification processes.
Billing Staff Overload
Many growing practices eventually reach a point where their internal billing staff cannot keep up with increasing administrative demands. Staff members may struggle to manage claim submissions, follow up on unpaid accounts, and handle patient billing simultaneously.
Expanding Medical Practices
As healthcare practices expand their services or patient volume, the complexity of the revenue cycle also increases. Implementing structured revenue cycle management ensures that financial operations scale effectively alongside clinical growth.
How Outsourcing RCM Improves Practice Revenue
Outsourcing revenue cycle management has become a common strategy for healthcare providers who want to improve efficiency and reduce administrative burdens. Experienced RCM teams bring specialized knowledge, technology, and compliance expertise to the billing process.
Access to Experienced Coders and Billing Experts
Professional revenue cycle teams include certified coders and billing specialists who understand payer guidelines and regulatory requirements. Their expertise helps prevent documentation errors and improve claim accuracy.
Stronger Denial Management
Outsourced RCM providers use structured denial tracking systems to identify recurring issues in claim processing. By addressing the root causes of denials, practices can recover lost revenue and improve clean claim rates.
Advanced Reporting and Compliance
Revenue cycle companies also provide detailed financial reporting and compliance monitoring. These insights help healthcare organizations track key performance indicators and maintain regulatory compliance.
Healthcare providers that partner with experienced billing and RCM specialists often see improvements in reimbursement speed, claim accuracy, and overall revenue stability.
Frequently Asked Questions
The difference between medical billing and revenue cycle management lies in their scope. Medical billing primarily involves submitting insurance claims, posting payments, and following up on denied claims. Revenue cycle management covers the entire financial process in healthcare, starting from patient registration and insurance verification to medical coding, claim submission, payment collection, and financial reporting. Medical billing is one part of the larger revenue cycle management process.
Yes, medical billing is a key component of revenue cycle management. Revenue cycle management includes several steps, such as patient registration, eligibility verification, medical coding, charge capture, claim submission, payment posting, denial management, and reporting. Medical billing specifically focuses on the claim submission and reimbursement stage within this broader workflow.
Revenue cycle management is important because it ensures healthcare providers receive accurate and timely payments for the services they deliver. A well-structured revenue cycle improves clean claim rates, reduces claim denials, shortens reimbursement timelines, and provides better financial visibility for medical practices. Effective RCM also helps identify operational issues that may be affecting revenue.
A practice can operate with only medical billing services, but it may face limitations in revenue optimization. Billing focuses on claim processing, while revenue cycle management addresses the full financial workflow. Without a complete revenue cycle strategy, practices may experience higher denial rates, delayed payments, and missed revenue opportunities.
A healthcare practice should consider full revenue cycle management when it experiences frequent claim denials, delayed reimbursements, increasing accounts receivable days, or billing staff overload. Growing practices also benefit from RCM because it provides structured workflows and financial insights that support long-term revenue stability.
Outsourcing revenue cycle management can improve collections by providing access to experienced billing specialists, certified medical coders, and advanced analytics tools. Professional RCM teams monitor claim accuracy, manage denials efficiently, and track key financial metrics, which helps healthcare providers improve reimbursement rates and reduce revenue leakage.
Final Thoughts
Understanding the difference between medical billing and revenue cycle management is important for healthcare providers who want to improve financial performance. Medical billing focuses on claim submission, reimbursement, and payment posting, while revenue cycle management covers the entire financial process from patient registration to final payment. When practices only focus on billing, they often miss opportunities to improve cash flow and reduce denials.
For small practices, a comprehensive revenue cycle strategy can improve claim accuracy, expedite reimbursements, and enhance financial visibility. Managing front-end processes, coding accuracy, and denial management together creates a more stable revenue flow.
If your practice is experiencing claim delays or high denial rates, Kaizen Systems can help with our Medical Billing Services, Medical Coding Services, and Credentialing Services, designed to strengthen your entire revenue cycle.



