Medical billing is not a single task. It follows a structured workflow with multiple steps, teams, and systems that work together to ensure accurate reimbursement. If anyone handles a step incorrectly, they can cause claim denials, delay payments, and lose revenue.
For healthcare practices, a clear, organized billing workflow is essential. It helps reduce errors, improve efficiency, and maintain consistent cash flow.
This guide walks through the complete billing workflow and explains how each step fits into the broader revenue cycle management process.
What Is the Medical Billing Workflow?
The billing workflow is the step-by-step process of managing patient billing from the moment a patient schedules an appointment to the final payment collection. It includes front-end activities such as patient registration, middle processes such as coding, and back-end tasks such as payment posting and denial management.
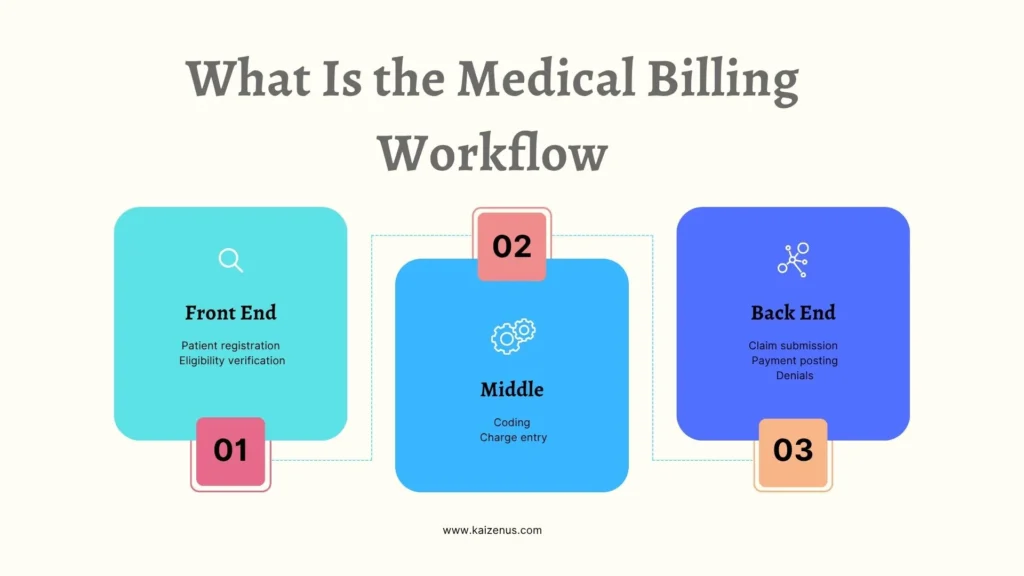
This workflow forms a core component of revenue cycle management. It connects administrative, clinical, and financial operations into one continuous system. Each stage plays a specific role and ensures healthcare providers receive accurate, timely reimbursement.
A well-defined healthcare billing workflow prevents confusion, coordinates teams, and keeps practices financially stable. When you clearly structure every step, you easily spot errors and boost overall performance.
Overview of the Billing Workflow Steps
Medical billing is the backbone of healthcare revenue. Before diving deeper, it is helpful to understand the full structure of the medical billing process. Each step builds on the previous one, making accuracy at every stage essential.
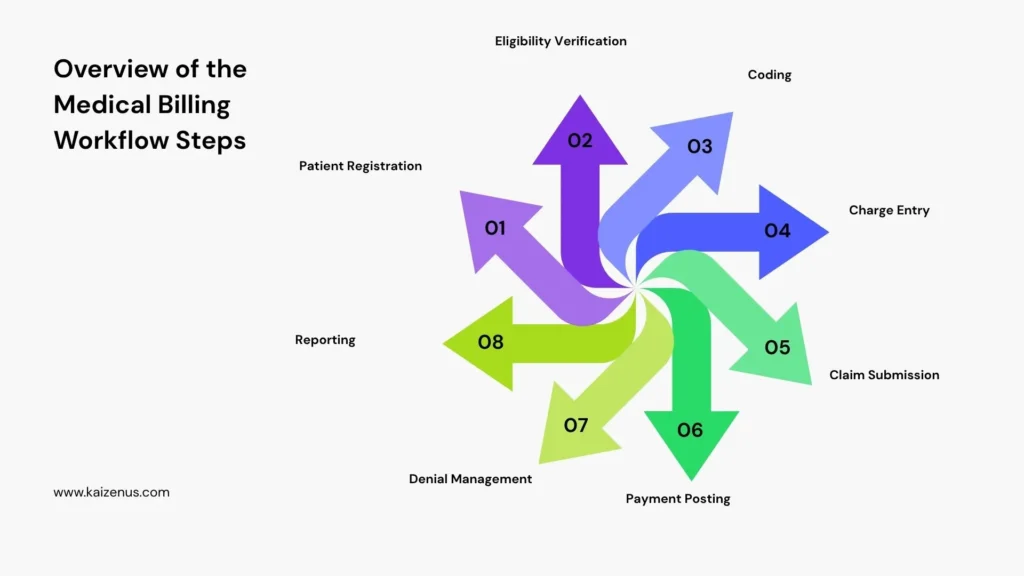
The main steps in medical billing cycle steps include:
- Patient Registration
- Insurance Eligibility Verification
- Medical Coding
- Charge Entry
- Claim Submission
- Payment Posting
- Denial Management
- Reporting and Analytics
Each step is vital in the revenue cycle workflow. When done right, they bring faster payments and fewer billing issues.
Step-by-Step Billing Workflow
Patient Registration
Patient registration begins the billing workflow and stands as one of the most important steps. During this stage, staff collect patient demographics (age, gender, address), contact details (phone number, email), and insurance information (insurer name, policy number).
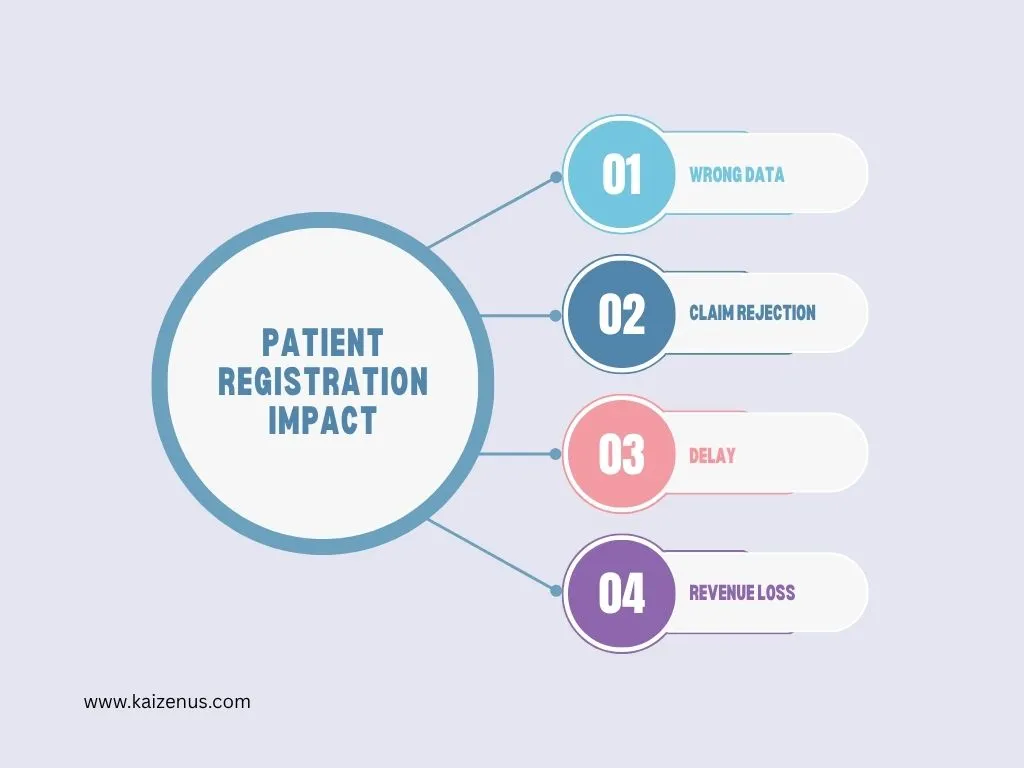
Accuracy at this stage is essential. Even small errors, such as incorrect name spelling or incorrect policy numbers, can lead to claim rejection later. Proper registration helps improve clean claim rates and reduces the need for rework.
As the registration process concludes, the next crucial step in the workflow is verifying the patient’s insurance eligibility.
Insurance Eligibility Verification
Insurance eligibility verification involves confirming that a patient’s insurance coverage is active and valid before services are provided. It also includes checking benefits (what services are covered), co-pay amounts (what the patient must pay at the time of care), deductibles (the amount the patient pays before insurance coverage begins), and service coverage (what specific treatments or procedures are covered by the plan).
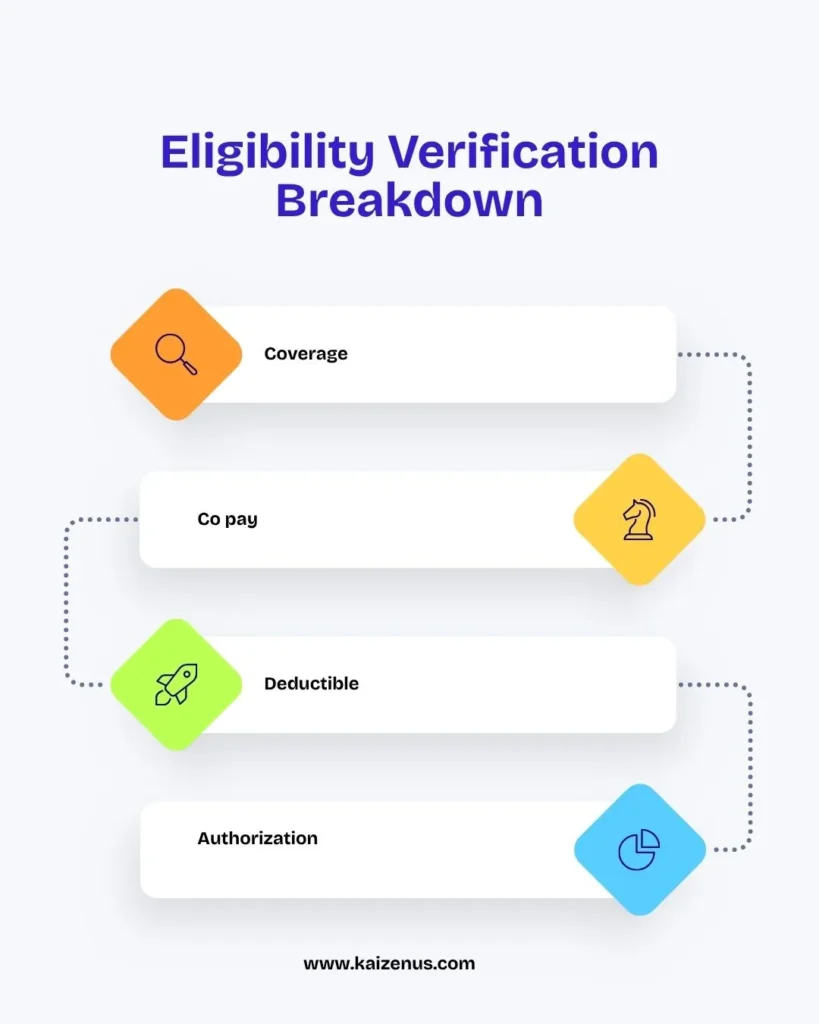
Verifying coverage in advance helps prevent claim denials and ineligible submissions.
With eligibility confirmed, attention turns to accurately coding the clinical services provided, which is the foundation for proper billing.
Medical Coding
Coders translate clinical services into standardized codes, such as CPT (Current Procedural Terminology) and ICD (International Classification of Diseases). Insurance companies use these codes to determine reimbursement.
Coding accuracy is essential for compliance and proper payment. Coding errors can lead to claim denials, underpayments, or audits.
Once coding is complete, these codes move to the charge entry phase, where accurate documentation ensures a seamless claim process.
Charge Entry
Staff enter coded services into the billing system. This step ensures proper documentation and billing for all services provided.
Billing teams review charges for accuracy and completeness during this stage. Missing or incorrect information can affect claim submission.
Entering charges properly ensures that claims show the correct services and support accurate reimbursement.
Claim Submission
After you enter charges, you submit claims (requests for payment) to insurance payers (companies that provide health insurance). Most practices use clearinghouses (third-party organizations that check claims for errors) to process claims and catch mistakes before submission.
A clean claim contains accurate information and needs no corrections. Submitting clean claims improves approval rates and speeds up payment.
Following claim submission, the focus shifts to payment posting as reimbursements are received and recorded in the billing system.
Payment Posting
Staff record payments received from insurance companies and patients during payment posting. This step keeps accounts accurately updated.
Staff reconcile payments with expected reimbursement amounts and quickly resolves any discrepancies.
Any issues identified during payment posting lead naturally to denial management, ensuring denied claims are handled promptly.
Denial Management
Denial management is the process of identifying, correcting, and resubmitting denied claims. It also involves analyzing patterns to prevent future denials.
Common reasons for denial include coding errors, missing information, and eligibility issues. Addressing these issues promptly helps recover revenue and improve efficiency.
To transition, refer to our guide on reducing claim denials in medical billing for a deeper understanding.
Reporting and Analytics
Reporting and analytics deliver insights into how the billing workflow performs. Key metrics track accounts receivable days (average days to collect payment), clean claim rate (percentage of claims accepted without corrections), and denial rate (percentage of claims rejected by payers).
By tracking these metrics, practices identify trends, measure efficiency, and make informed decisions. Teams can also address issues before they impact revenue. Strong reporting systems are essential for optimizing the overall revenue cycle.
Common Challenges in the Billing Workflow
Many healthcare practices encounter obstacles that undermine the efficiency of their billing workflows. These disruptions frequently result in delayed reimbursements, denied claims, and lost revenue.
For example, data entry errors are one of the most common problems. Incorrect patient information can cause claims to be rejected immediately. In addition, coding mistakes often result in denied or underpaid claims.
Delayed claim submission hampers reimbursement and extends accounts receivable days. Inadequate follow-up on unpaid claims results in lost revenue opportunities.
Insufficient reporting hinders pinpointing issues and boosting performance. Lacking access to key metrics, practices cannot make data-driven decisions.
Addressing these challenges is essential to maintaining a smooth, efficient billing process.
How to Optimize Your Billing Workflow
Optimizing billing workflows is crucial for practices aiming to improve financial health and operational efficiency. By implementing structured processes, consistent training, and technology solutions, practices can reduce errors, improve revenue cycles, and position themselves for long-term success.
Standardize Processes
Establish standardized workflows to ensure consistency in all billing activities. This approach limits variability and compels staff to follow best practices at all times.
Train Staff Regularly
Mandate ongoing training so staff remain current on billing regulations, coding guidelines, and payer requirements. Well-trained teams consistently minimize errors.
Use Billing Software
Implement modern billing software to automate core tasks, eliminate manual errors, and drive efficiency. Real-time data empowers informed, strategic decisions.
Monitor KPIs
Track crucial performance indicators such as clean claim rates and accounts receivable days without exception. These metrics reveal both successes and areas needing improvement.
Improve Communication
Implement these strategies today to streamline your billing workflow and boost your financial performance.
How an Efficient Workflow Improves Revenue Cycle Performance
An efficient billing workflow directly impacts revenue cycle management. When each step is performed accurately and on time, claims are processed faster, and payments are received sooner.
With fewer errors, claim denials decrease. As a result, staff spend less time on corrections and resubmissions, which raises productivity and eases administrative workload.
The speed of reimbursement contributes to better cash flow and greater financial stability. Additionally, patients benefit from billing that is clear and accurate, leading to an improved overall experience.
By supporting better financial outcomes, a strong workflow enables practices to operate more effectively.
How Outsourced Medical Billing Services Improve Workflow Efficiency
Small practices often face challenges with billing workflows due to limited staff. Outsourced medical billing services address these challenges with expert support at every step.
Professional billing teams use advanced tools and proven workflows to ensure accuracy at every stage. They help reduce errors, improve claim acceptance rates, and speed up processing times.
Outsourcing also provides access to detailed reporting and analytics, allowing practices to monitor performance and make informed decisions.
At Kaizen Systems, our experienced team leverages industry expertise, innovative technology, and customized processes to deliver tailored medical billing, coding, and revenue cycle management solutions. These distinct capabilities streamline workflows and maximize revenue for healthcare practices.
Frequently Asked Questions
The main steps include patient registration, insurance verification, medical coding, charge entry, claim submission, payment posting, denial management, and reporting.
The process length varies, but efficient workflows speed up billing.
Every step is important, but accurate patient registration and precise coding directly influence claim acceptance rates and reimbursement, making them especially impactful.
Standardizing processes, training staff, and implementing advanced billing software help reduce errors.
Outsourcing provides expert support, reduces errors, and increases overall billing performance.
Final Words
The medical billing workflow drives healthcare operations. Each step, from patient registration to final payment, directly affects the speed and accuracy of provider reimbursement.
When workflows are structured and optimized, practices can reduce errors, minimize claim denials, and improve cash flow. On the other hand, inefficiencies at any stage can lead to delays and revenue loss.
Healthcare practices aiming to improve financial performance should take decisive action to strengthen their billing processes.
Consider partnering with experienced professionals to drive results. Contact Kaizen Systems today to discover how our medical billing services, coding services, and revenue cycle management services can streamline your workflow and help you achieve better financial outcomes.



