Billing errors in healthcare escalate quickly. A missed modifier, incomplete documentation, or incorrect code can quickly lead to denied claims, delayed payments, and compliance risks. Many practices do not realize the impact until revenue drops or an audit is triggered.
A structured medical billing audit catches these issues early and keeps your processes aligned with payer rules. It forms a critical part of strong revenue cycle management. When you audit consistently, you improve accuracy, protect revenue, and reduce risk.
This guide explains how the medical billing audit process works and why it is essential for compliance and financial performance.
What Is a Medical Billing Audit?
A medical billing audit is a systematic review of billing activities, coding, and claim submissions. It ensures services are properly documented and billed in line with payer and regulatory requirements.
Auditors examine patient records, verify coding, and review claims to identify errors or inconsistencies. Their goal is to ensure billing accuracy, regulatory compliance, and appropriate reimbursement.
There are two main types of audits. Internal audits are conducted by your team to monitor performance regularly. External audits are performed by independent experts who provide an objective assessment of billing practices.
Both types support compliance and improve billing efficiency within your practice.
Types of Medical Billing Audits
Each audit type addresses a specific aspect of the billing process. Understanding these options helps you select the most effective approach for your practice.
Internal Audits
Your staff conducts internal audits regularly to identify issues early and implement continuous improvements.
External Audits
External audits are conducted by independent experts. They provide an objective review of your billing, often focusing on compliance or preparing for regulatory reviews.
Prospective Audits
Teams conduct prospective audits before submitting claims. This helps catch mistakes early and prevent claim denials.
Retrospective Audits
Teams do retrospective audits after claims are submitted. These audits look for patterns, help recover lost revenue, and fix past errors.
The Medical Billing Audit Process
Having a solid audit process in place is key if you want to keep things consistent and accurate. Each step is there to help you spot problems early and actually fix them before they turn into bigger headaches.
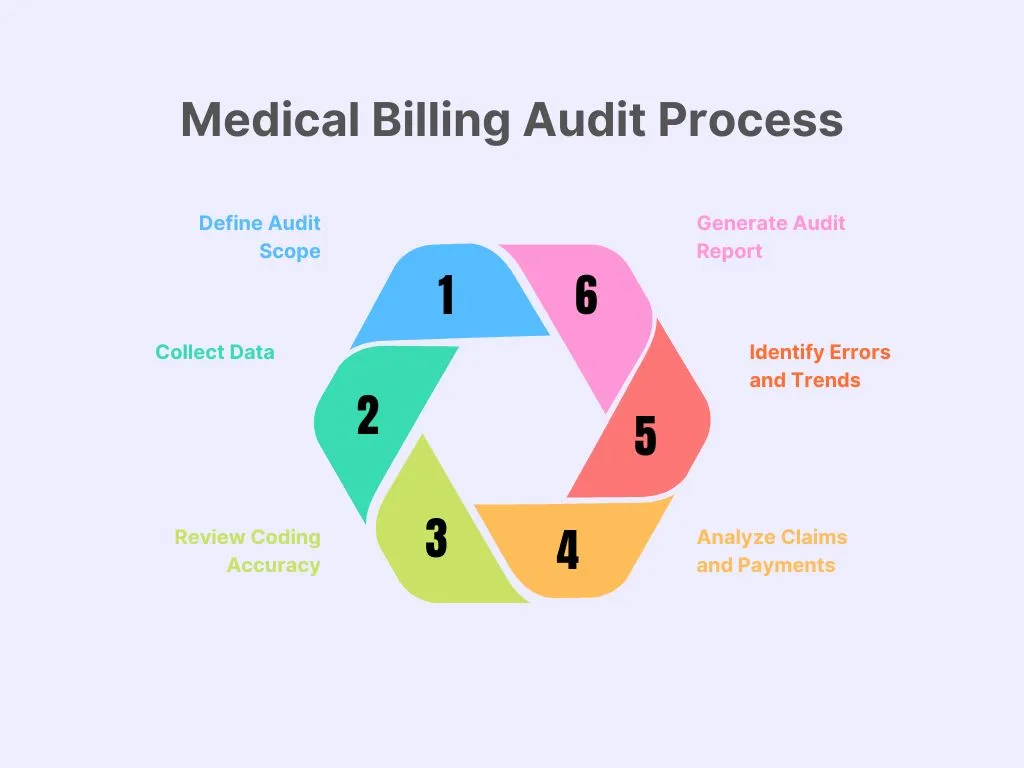
Step 1: Define Audit Scope
Start by figuring out exactly what you want to look at in your audit. Are you checking coding accuracy, claim submissions, documentation quality, or maybe focusing on a certain department? Getting clear on your scope up front saves you time and keeps your audit on track.
Step 2: Collect Data
Pull together all the data you’ll need—patient records, billing reports, claim histories, you name it. If your data isn’t accurate, you’re not going to get a true picture of what’s going on.
Step 3: Review Coding Accuracy
Take a close look at your CPT codes, ICD codes, and modifiers to make sure they actually match what’s in the documentation. This is where you’ll catch coding mistakes and spot any healthcare billing compliance risks before they cause trouble.
Step 4: Analyze Claims and Payments
Go through your claims and see where you’re getting denials, underpayments, or payment delays. These are usually signs that there are gaps in your revenue process that need to be fixed.
Step 5: Identify Errors and Trends
Break down any issues that keep popping up so you can figure out what’s really causing them. Spotting these trends helps you zero in on weak spots in your process.
Step 6: Generate Audit Report
The final report summarizes findings, highlights risks, and offers recommendations for improvement. This report serves as the basis for corrective action.
Common Errors Found in Medical Billing Audits
When you carry out audits, you’ll usually spot patterns in the errors that can hurt both compliance and your bottom line. Catching these early makes it a lot easier to prevent bigger problems down the road.
Incorrect Coding
If you get CPT or ICD codes wrong, you’re likely to see claim denials or end up getting paid the wrong amount.
Missing Documentation
Incomplete clinical notes do not support billed services, leading to rejected claims.
Duplicate Billing
Sending in duplicate claims is a surefire way to get rejections from payers and raise compliance red flags.
Upcoding or Undercoding
If you code services at the wrong level, you’re not just risking compliance issues—you’re also leaving money on the table.
Eligibility or Authorization Issues
If you skip insurance verification or don’t get the right authorizations, you’ll end up with denied claims. Most of the time, these problems come from missing steps in your eligibility and authorization process.
Why Medical Billing Audits Are Important for Compliance
Medical billing audits are essential for maintaining compliance with healthcare regulations and payer requirements. They help catch issues early and ensure your billing meets current standards.
Skipping audits invites costly compliance trouble such as penalties, takebacks, or legal action. Even honest mistakes can cause problems.
Audits provide transparency and accountability. They provide documentation to support billing and demonstrate your commitment to compliance.
When you build your revenue cycle audit, you shore up your processes and cut down on risk throughout your billing workflow.
How Audits Improve Revenue Cycle Performance
Audits aren’t just about checking boxes for compliance. They actually help boost your bottom line.
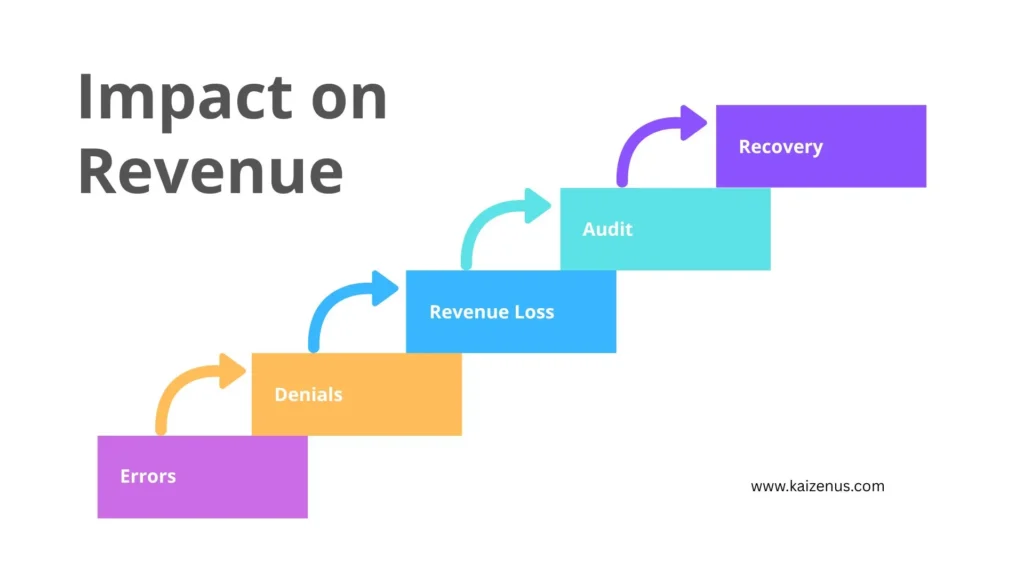
One big win is cutting down on claim denials. When you spot errors early through audits, you can fix them before the claim ever goes out the door.
Audits also help you bump up your clean claim rate. The more accurate your claims, the faster they get processed and paid.
Audits help increase revenue by identifying underpayments and missed billing opportunities. They also highlight process gaps that can be corrected to improve efficiency.
At the end of the day, regular audits set you up for a stronger revenue cycle and better financial results.
How Often Should Medical Billing Audits Be Conducted
How often you should run billing audits really comes down to how big your practice is and how complicated your billing gets.
High-volume practices benefit from monthly audits. Frequent reviews help manage large claim volumes and reduce error rates.
For smaller practices, quarterly audits usually strike the right balance. You’ll still keep an eye on your billing without stretching your team too thin.
At the very least, make sure you’re doing a full audit once a year. This helps you stay compliant and spot any bigger issues that might be building up over time.
No matter how often you do them, regular audits are key if you want to keep your billing accurate and your practice running smoothly.
Best Practices for Effective Medical Billing Audits
Following best practices ensures audits are effective and actionable.
Use Standardized Audit Checklists
Using a checklist keeps your audits consistent and makes sure you don’t miss any important steps along the way.
Train Staff Regularly
Keep your team trained up on the latest coding rules and billing requirements. When everyone’s up to speed, you’ll see fewer mistakes in the long run.
Monitor Key Metrics
Keep an eye on your key numbers, like denial rates and clean claim rates. Watching these metrics gives you a real sense of how your billing is performing.
Implement Corrective Actions
Don’t just file your audit results away. Use them to fix what’s not working. Tackling issues head-on now helps you avoid the same mistakes popping up again.
How Outsourced Medical Billing Services Support Audits
Outsourcing your audits lets you access a team that knows billing inside and out. These professionals bring real expertise and proven processes to catch mistakes and keep your numbers accurate.
They dig into your coding, claims, and documentation with a fine-tooth comb. This approach lets you spot issues you might miss when you look at things in-house.
Outsourced billing teams stay on top of all the changing rules and payer requirements, so you avoid falling behind. They monitor your processes and send you regular updates, letting you see where things improve.
At Kaizen Systems, we don’t treat audits as a one-off task. We build them right into your whole billing and revenue cycle plan. This approach helps your practice stay compliant, cut down on errors, and see real improvements in how you get paid.
Frequently Asked Questions
A medical billing audit checks billing, coding, and claims for accuracy and compliance.
They catch errors, prevent denials, and ensure compliance.
Monthly for large, quarterly for small, or annually for all practices.
Common errors include incorrect coding, missing documentation, duplicate billing, and authorization issues.
Yes. Outsourcing means expert review and up-to-date compliance.
Final Words
Regular medical billing audits help you maintain compliance and protect your revenue. Even small mistakes can quickly snowball into big financial headaches or compliance problems if you miss them early.
When you make audits a regular part of your routine, you catch problems before they turn into bigger issues. This not only helps you bill more accurately, but also keeps your practice running smoothly and boosts your bottom line.
If you’re dealing with denials, billing mistakes, or you just feel unsure about compliance, you need to dig into your billing processes. Working with a knowledgeable team helps you set up solid audits, tighten your accuracy, and build a revenue cycle that works for you in the long run.



