Many claim denials do not start at the billing stage. They begin much earlier, often before a patient even receives care. One of the most common reasons is missing or incorrect prior authorization. When this step is overlooked, practices face delayed payments, denied claims, and frustrated patients.
Think of prior authorization in medical billing as the foundation of front-end revenue cycle management. By securing approvals upfront, you pave the way for smoother operations.
In this guide, you’ll discover what prior authorization really involves, how each step unfolds, and why mastering this process is key to better reimbursement and financial health.
What Is Prior Authorization in Medical Billing?
Prior authorization in medical billing refers to the approval required from an insurance payer before certain medical services are performed. Without this approval, the payer may refuse to cover the service, even if it is medically necessary.

This requirement is typically applied to high-cost procedures, advanced imaging, specialist visits, or specific medications. Insurance companies use prior authorization to confirm that the proposed treatment meets medical necessity guidelines.
By confirming coverage and medical necessity beforehand, prior authorization also helps ensure that services are covered under the patient’s policy. If authorization is not obtained in advance, the provider may not be reimbursed, leading to revenue loss and additional administrative work.
Why Prior Authorization Is Required by Insurance Companies?
Insurance companies require prior authorization to manage costs and maintain control over healthcare spending. By evaluating whether a treatment is appropriate before approving payment, they seek to ensure resources are used wisely.

In addition to cost management, one key purpose is cost control. By reviewing services beforehand, payers can prevent unnecessary or overly expensive procedures. This process lowers overall healthcare costs. It also ensures efficient resource use.
Furthermore, another reason is policy compliance. Each insurance plan has specific coverage rules. Prior authorization ensures that the requested service aligns with these guidelines.
It also supports quality of care by encouraging evidence-based treatments. While it may seem like an administrative burden, it helps maintain consistency across healthcare services.
The Prior Authorization Process in Healthcare
You must complete several steps in the prior authorization process accurately to avoid delays or denials.
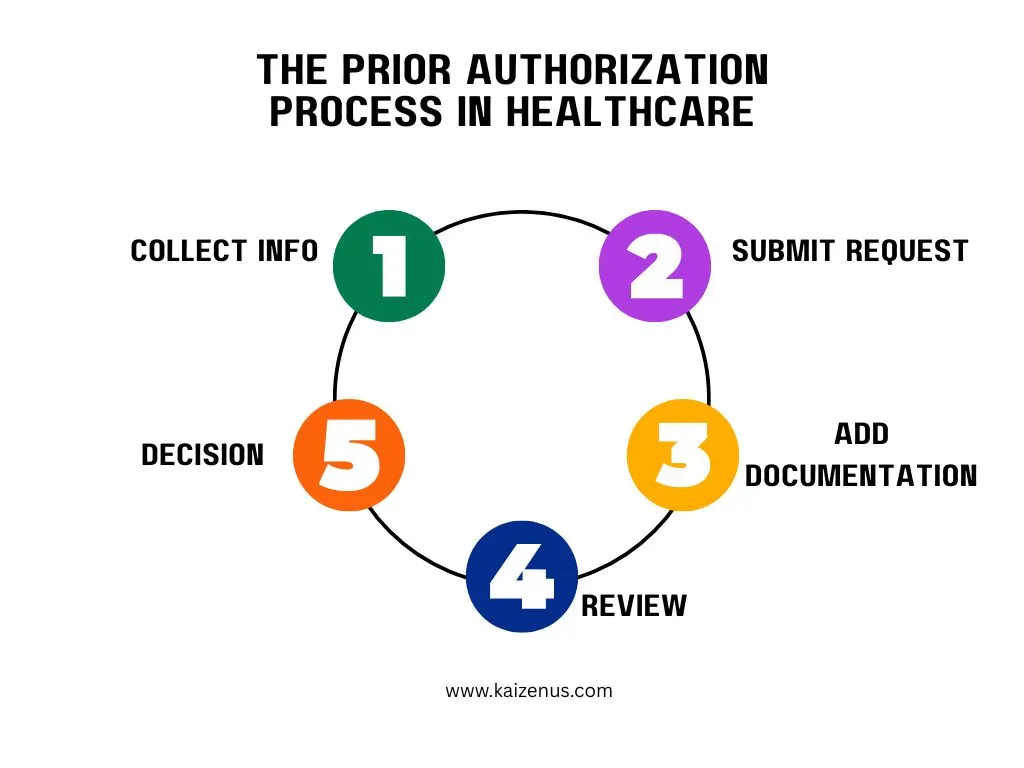
Identify Services Requiring Authorization
Begin by identifying which services require prior authorization. These may include surgeries, imaging procedures, or specialist consultations. Always review payer guidelines carefully, as requirements vary.
Collect Patient and Insurance Information
Collect accurate patient demographics and insurance details. Errors at this stage can cause rejected authorization requests and delay care.
Submit Authorization Request
You can submit the request through payer portals, fax, or clearinghouse systems. Submit on time to prevent treatment delays.
Provide Clinical Documentation
Include supporting clinical documentation such as physician notes, test results, and treatment plans to justify medical necessity.
Receive Approval or Denial
The payer reviews the request and responds with approval, denial, or a request for more information. Follow up promptly to keep the process moving.
The Prior Authorization Process in Healthcare
You must complete several steps in the prior authorization process accurately to avoid delays or denials.
Identify Services Requiring Authorization
Identify which services require prior authorization. Review payer guidelines carefully, as requirements vary.
Collect Patient and Insurance Information
Collect accurate patient demographics and insurance details. Avoid errors to prevent rejected requests and delayed care.
Submit Authorization Request
Submit the request through payer portals, fax, or clearinghouse systems on time to prevent treatment delays.
Provide Clinical Documentation
To justify medical necessity, include supporting clinical documentation such as physician notes, test results, and treatment plans.
Receive Approval or Denial
Once submitted, the payer reviews the request and responds with approval, denial, or a request for more information. Follow up promptly to keep the process moving.
How Prior Authorization Impacts Reimbursement
Prior authorization has a direct impact on whether and when a practice gets paid. Even a small mistake can lead to significant revenue loss.
If authorization is not obtained, the claim is likely to be denied. This means the provider will not receive payment for the service.
Delayed authorization leads to delayed reimbursement. Payments cannot be processed until approval is confirmed.
Incorrect authorization can result in partial payments or claim rejection. For example, if the approved service does not match the billed procedure, the payer may deny the claim.
This is why prior authorization is closely tied to revenue cycle performance. It affects claim accuracy, payment timelines, and overall financial stability.
Prior Authorization Denials and Their Causes
Prior authorization-related denials are common and often preventable. Understanding the root causes helps reduce these issues.
A major cause is missing authorization. Without the required approval obtained in advance of the service, the claim will be denied.
Expired authorization is another issue. Authorizations are valid for a limited time. If services are performed after the expiration date, reimbursement may be denied.
A mismatch between service and approval can also lead to rejection. The billed procedure must match the approved service exactly.
Incorrect coding is also a factor, as coding errors can invalidate an authorization and result in a denial.
To understand how these issues connect to broader billing problems, it is helpful to review strategies for reducing claim denials in medical billing.
Best Practices to Manage Prior Authorization Efficiently
Improving prior authorization processes can significantly reduce delays and denials.
Verify Authorization Requirements Early
Always check authorization requirements before scheduling services. Early verification prevents last-minute issues.
Standardize Authorization Workflow
Create a clear workflow for handling authorization requests. This ensures consistency and reduces errors.
Maintain Updated Payer Guidelines
Keep track of payer policies and updates. This helps avoid mistakes caused by outdated information.
Use Tracking Systems
Implement systems to monitor authorization requests. Tracking ensures timely follow-up and prevents missed approvals.
Train Staff Regularly
Staff training is essential for accuracy. Well-trained teams can handle authorization requirements more efficiently.
How Technology Improves the Prior Authorization Process
Technology streamlines prior authorization by automating verification and rapid submission of requests.
Real-time payer systems allow practices to check authorization status instantly. This reduces waiting time and improves workflow efficiency.
Automation takes the stress out of manual data entry. By reducing errors, you get more accurate results and spend less time on corrections.
Advanced systems seamlessly connect with billing platforms, letting you enjoy a smooth journey from verification right through to claim submission.
How Outsourced Medical Billing Services Handle Prior Authorization
For this reason, many practices choose to outsource prior authorization to improve efficiency and reduce administrative burden.
Outsourced teams become your authorization experts. They know payer rules and use efficient, structured processes for accuracy every time.
Dedicated staff manage submissions, track approvals, and handle follow-ups. This leads to faster processing and fewer delays.
Outsourcing also improves compliance. Experienced teams stay up to date on changing payer rules and documentation requirements.
At Kaizen Systems, prior authorization seamlessly integrates into our end-to-end billing and revenue cycle strategy, reducing denials and supporting your ongoing reimbursement goals.
Frequently Asked Questions
Approval from an insurer is required before certain services.
High-cost procedures, imaging, specialist visits, and some medications.
The claim is likely to be denied, and the provider may not receive payment.
It can take anywhere from a few hours to several days, depending on the payer and service.
Verify early, use tracking, and document accurately.
Conclusion
Prior authorization directly impacts billing outcomes. When you handle it properly, you get services approved, reduce claim denials, and receive reimbursement faster.
Delays, errors, or missed authorizations disrupt the revenue cycle and cause financial losses. Strong front-end processes prevent these issues in every healthcare practice.
Take action now: review your prior authorization workflows or consult with a billing expert to address delays and denials. Strengthen your processes today to ensure steady and consistent revenue for your practice.



